Influence of intimate hair removal on the appearance of vaginal and urinary tract infections. Cross-sectional study
DOI:
https://doi.org/10.29176/2590843X.1664Abstract
Objective: To evaluate the influence of intimate hair removal on the appearance of vulvo-vaginal and urinary (genitourinary) infections.
Materials and methods: Cross-sectional study. 861 women over 18 years of age, with the habit of intimate hair removal, who attended the outpatient gynecology consultation, residing in Quindío, Colombia, in three highly complex clinics were included, between 2014 and 2019. The diagnosis of bacterial vaginosis was established using the Nugent score, vaginitis (candidiasis and/or trichomonas) by direct smear in wet and urinary infection by urine culture. Data associated with the time of epilation practice, presence of genitourinary infections, as well as the prevalence were related.
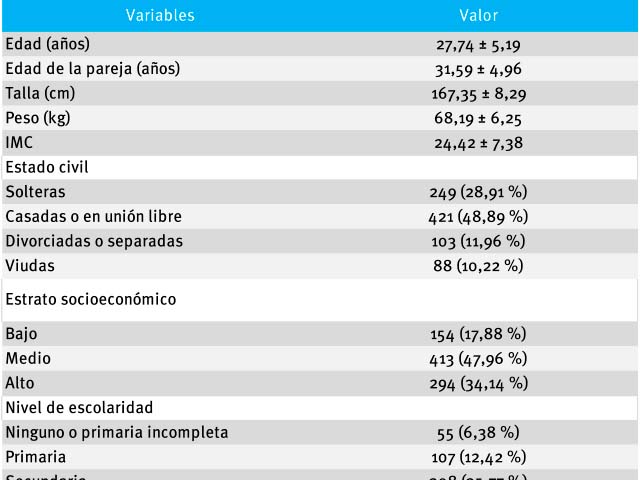
Results: The mean age of the population was 27.74 ± 5.19 years. 29.96% of the women had been waxing for a period of more than 5 years and less than 10 years; 62.36% reported 10 years or more, and 7.66% less than 5 years. 84.43% presented genitourinary infections, of which 41.95% were vaginal infections; 27.37% urinary infections, and 30.67 vaginal and urinary infections concomitantly. A statistically significant relationship was observed between hair removal time greater than 5 years and the appearance of genitourinary infections (p = 0.001; odds ratio [OR] = 5.79; 95% CI: 1.89-7.35). Higher risk was found among women who used long pants, tampon users and those who did not use cotton underwear (OR = 6.92; 95% CI: 1.11-15.28).
Conclusions: There is a relationship between intimate hair removal and the appearance of vulvo-vaginal and/or urinary infections. Future research should confirm these findings, as well as the influence of different hair removal methods that were associated with more or less infection.
Author Biography
Franklin José Espitia De La Hoz, Ginecología y Obstetricia / Universidad Militar nueva Granada Sexología Clínica - Máster en sexología: educación y asesoramiento sexual / Universidad de Alcalá de Henares Uroginecología / FUCS - Hospital de San José / Unicamp, Brasil.Director Científico: Hathor, Clínica Sexológica.
Ginecología y Obstetricia / Universidad Militar nueva Granada Sexología Clínica - Máster en sexología: educación y asesoramiento sexual / Universidad de Alcalá de Henares Uroginecología / FUCS - Hospital de San José / Unicamp, Brasil.Director Científico: Hathor, Clínica Sexológica.
References
Espitia-De La Hoz FJ. Sexo ilimitado/El vuelo hacia una sexualidad más placentera. Bogotá. Editorial Bolívar; 2015.
Ramsey S, Sweeney C, Fraser M, Oades G. Pubic hair and sexuality: A review. J Sex Med. 2009;6(8):2102-10. https://doi.org/10.1111/j.1743-6109.2009.01307.x
Dendle C, Mulvey S, Pyrlis F, Grayson ML, Johnson PD. Severe complications of a “Brazilian” bikini wax. Clin Infect Dis. 2007;45(3):e29-31. https://doi.org/10.1086/519425
Labre MP. The Brazilian wax: New hairlessness norm for women? J Comm Inq. 2002;26:113-32. https://doi.org/10.1177/0196859902026002001
Glass AS, Bagga HS, Tasian GE, Fisher PB, McCulloch CE, Blaschko SD, et al. Pubic hair grooming injuries presenting to US emergency departments. Urology. 2012;80(6):1187-91. https://doi.org/10.1016/j.urology.2012.08.025
Castronovo C, Lebas E, Nikkels-Tassoudji N, Nikkels AF. Viral infections of the pubis. Int J Std Aids. 2012;23:48-50. https://doi.org/10.1258/ijsa.2011.010548
Chang AC, Watson KM, Aston TL, Wagstaff M, Greenwood J. Depilatory wax burns: experience and investigation. Eplasty. 2011;11:e25.
Díaz-Martínez LA. Contextualización histórica y social de la remoción del vello púbico femenino. Rev Colomb Obstet Ginecol. 2013;64(4):327-32. https://doi.org/10.18597/rcog.92
DeMaria AL, Berenson AB. Prevalence and correlates of pubic hair grooming among low-income Hispanic, Black, and White women. Body Image. 2013;10(2):226-31. https://doi.org/10.1016/j.bodyim.2013.01.002
Herbenick D, Schick V, Reece M, Sanders S, Fortenberry D. Pubic hair removal among women in the United States: prevalence, methods, and characteristics. J Sex Med. 2010;7(10):3322-30. https://doi.org/10.1111/j.1743-6109.2010.01935.x
Begier EM, Frenette K, Barrett NL, Mshar P, Petit S, Boxrud D, et al. A high-morbidity outbreak of methicillin-resistant Staphylococcus aureus among players on a college football team, facilitated by cosmetic body shaving and turf burns. Clin Infect Dis. 2004;39(10):1446-53. https://doi.org/10.1086/425313
Roth LM, Look KY. Inverted follicular keratosis of the vulvar skin: a lesion that can be confused with squamous cell carcinoma. Int J Gynecol Pathol. 2000;19(4):369-73. https://doi.org/10.1097/00004347-200010000-00012
Kolmos HJ, Svendsen RN, Nielsen SV. The surgical team as a source of postoperative wound infections caused by Streptococcus pyogenes. J Hosp Infect. 1997;35(3):207-14. https://doi.org/10.1016/s0195-6701(97)90208-5
Sladden MJ, Johnston GA. Current options for the treatment of impetigo in children. Expert Opin Pharmacother. 2005;6(13):2245-56. https://doi.org/10.1517/14656566.6.13.2245
Espitia De La Hoz FJ. Evaluación de la eficacia y seguridad del policresuleno en el tratamiento de la vaginitis mixta, Armenia, Colombia, 2017-2019. Estudio aleatorizado. Arch Med (Manizales). 2021;21(1):45-56. https://doi.org/10.30554/archmed.21.1.3756.2021
How to Cite
Downloads
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2021 Revista de la Asociación Colombiana de Dermatología y Cirugía Dermatológica

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.

| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |






