The great imitator: dermatologic features related to T. pallidum infection, a narrative review of the literature
DOI:
https://doi.org/10.29176/2590843X.1695Keywords:
Chancres, Cutaneous syphilis, Latent syphilis, Sexually transmitted diseases, Syphilis, Treponema pallidumAbstract
Introduction: syphilis is caused by T. pallidum, a sexually transmitted infection. Its main manifestations occur early at the dermatological level with numerous findings, the vast majority nonspecific.
Methods: Information was searched in Pubmed/Medline, ScienceDirect, JAMA and SciELO. 185 references were acquired, of which 65 were selected, to finally condense the information as a narrative review of the literature.
Results: The syphilitic chancre is the primary manifestation, however, extragenital manifestations that could go unnoticed are also described. The secondary and tertiary stages include maculopapular outbreaks, plaques and nodular forms, mimicking other dermatoses.
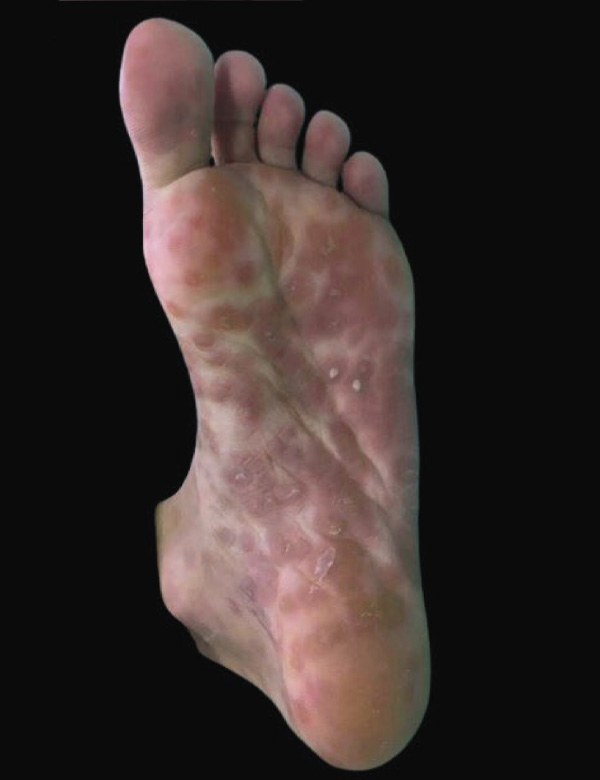
Conclusion: Syphilis is considered the great imitator. Maculopapular eruptions with palmoplantar involvement should always be considered as a differential diagnosis, since if they are allowed to progress, considerable multisystem involvement is generated.
Author Biographies
Luis Daniel Pérez Cáceres, Fundación Universitaria Sanitas, Bogotá D.C.
Médico, Universidad Pedagógica y Tecnológica de Colombia - UPTC, Tunja Boyacá. Residente de Dermatología, Fundación Universitaria Sanitas, Bogotá D.C.
Miguel Mateo Cuervo, Universidad de Antioquia, Medellín, Colombia.
Médico dermatólogo, Universidad de Antioquia. Hospital Alma Máter de Antioquia. Docente, Universidad de Antioquia.
References
Peeling, R., Mabey, D., Kamb, M., Cheng, X., Radolf, J., Benzaken, A. Syphilis. Nat Rev Dis Primers. 2017; 3: 1-21. DOI: https://doi.org/10.1038/nrdp.2017.73
Ros-Vivancos, C., González-Hernández, M., Navarro-Gracia, J. F., Sánchez-Payá, J., González-Torga, A., & Portilla-Sogorb, J. Evolución del tratamiento de la sífilis a lo largo de la historia. Rev Esp Quimioter 2018; 31(6): 485-492. PMID: 30427145
Willeford, W.G., Bachmann, L.H. Syphilis ascendant: a brief history and modern trends. Trop Dis Travel Med Vaccines, 2016; 2: 20. DOI: https://doi.org/10.1186/s40794-016-0039-4
Neira-Varillas, M., Donaires-Toscano, L. Sífilis materna y complicaciones durante el embarazo. An Fac med. 2019;80(1):68-72. DOI: https://doi.org/10.15381/anales.v80i1.15875
Balagula, Y., Mattei, P.L., Wisco, O.J., Erdag, G. and Chien, A.L. The great imitator revisited: the spectrum of atypical cutaneous manifestations of secondary syphilis. Int J Dermatol, 2014; 53: 1434-1441. DOI: https://doi.org/10.1111/ijd.12518
Patton ME, Su JR, Nelson R, Weinstock H. Primary and secondary syphilis - United States, 2005-2013. MMWR Morb Mortal Wkly Rep. 2014; 63(18):402-406. PMID: 24807239
Rowley J., Vander-Hoorn S., Korenromp E., Low N., Unemo M., Abu-Raddad LJ., et. al. Chlamydia, gonorrhoea, trichomoniasis and syphilis: global prevalence and incidence estimates, 2016. Bull World Health Organ. 2019 Aug 1;97(8):548-562P. DOI: 10.2471/BLT.18.228486.
Cáceres Karen. Situación epidemiológica de sífilis. Rev. chil. infectol. 2018; 35 (3): 284-296. DOI: http://dx.doi.org/10.4067/s0716-10182018000300284
World Health Organization. The Global Health Observatory: data on syphilis, men who have sex with men and syphilis; fecha de publicación 2020/07/2021, fecha de consulta: 2022/02/20. https://www.who.int/data/gho/data/themes/topics/topic-details/GHO/data-on-syphilis
Wandeler, G., Johnson, L. F., Egger, M. Trends in life expectancy of HIV-positive adults on antiretroviral therapy across the globe: comparisons with general population. Current opinion in HIV and AIDS. 2016, 11(5), 492–500. DOI: https://doi.org/10.1097/COH.0000000000000298
Centers for Disease Control and Prevention. Sexually Transmitted Disease Surveillance 2018. Atlanta: U.S. Department of Health and Human Services; 2019. DOI: 10.15620/cdc.79370.
Zoni, A. C., González, M. A., Sjögren, H. W. Syphilis in the most at-risk populations in Latin America and the Caribbean: a systematic review. Int J Infect Dis. 2013 Feb;17(2):e84-92. DOI: 10.1016/j.ijid.2012.07.021
Report on global sexually transmitted infection surveillance. Prevalence of syphilis among key populations. World Health Organization. ISBN 978-92-4-156569-1. 2018
Blandón-Buelvas, M., Palacios-Moya L., Berbesí-Fernández, D. Infección activa por sífilis en habitantes de calle y factores asociados. Rev. Salud Pública. 2019; 21(3): 1-5. DOI: https://doi.org/10.15446/rsap.V21n3.61039.
Galindo, J., Miranda, C.A., Rivas, J.C. Neurosífilis: un problema antiguo que no pierde actualidad. Rev colomb psiquiat. 2017; 46 (S1): 69–76. DOI: http://dx.doi.org/10.1016/j.rcp.2017.05.002
Comportamiento de sífilis gestacional y sífilis congénita. Boletín Epidemiológico Semanal, semana epidemiológica 30 del 19 al 25 de julio de 2020. Instituto Nacional de Salud. Ministerio de Salud Colombia. Páginas 2 - 4.
Meng Yin Wu, Hui-Zi G., Kui-Ru H., He-yi Z., Xia W., Jun L. Effect of syphilis infection on HIV acquisition: a systematic review and meta-analysis. Sex Transm Infect 2020; 0:1–9. doi:10.1136/sextrans-2020-054706
Jarzebowski W., Caumes E., Dupin N., Farhi D., Lascaux A.S., Piketty C., et.al. Effect of early syphilis infection on plasma viral load and CD4 cell count in human immunodeficiency virus-infected men: results from the FHDH-ANRS CO4 cohort. Arch Intern Med. 2012; 172(16): 1237-43. DOI: 10.1001/archinternmed.2012.2706.
Liu J., Howell J.K., Bradley S.D., Zheng Y., Zhou Z.H., Norris S.J.. Cellular Architecture of Treponema pallidum: Novel Flagellum Periplasmic Cone, and Cell Envelope as Revealed by Cryo-Electron Tomography. J Mol Biol. November 2010; 403 (4): 546-561. DOI: 10.1016/j.jmb.2010.09.020.
Smajs, D., Norris, S. J., Weinstock, G. M. Genetic diversity in Treponema pallidum: Implications for pathogenesis, evolution and molecular diagnostics of syphilis and yaws. Infectar Genet Evol. 2012; 12 (2): 191-202. DOI: 10.1016/j.meegid.2011.12.001.
Giacani L., Lukehart S.A., The endemic treponematoses. Clin Microbiol Rev 2014; 27: 89–115. DOI: 10.1128/CMR.00070-13.
Seña A.C., White B.L., Sparling P.F.. Novel Treponema pallidum serologic tests: a paradigm shift in syphilis screening for the 21st century. Clin Infect Dis. 2010; 51(6): 700-708. DOI: 10.1086/655832.
Salazar, J. C., Cruz, A. R., Pope, C. D., Valderrama, L., Trujillo, R., Saravia, N. G., et. al. Treponema pallidum Elicits Innate and Adaptive Cellular Immune Responses in Skin and Blood during Secondary Syphilis: A Flow‐Cytometric Analysis. The Journal of Infectious Diseases, 2007; 195(6), 879–887. DOI: 10.1086/511822
Tudor M.E., Aboud A.M., Gossman W. Syphilis. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 30521201. Bookshelf ID: NBK534780
Ghanem, K. G., Ram, S.,Rice, P. A. The Modern Epidemic of Syphilis. N Engl J Med. 2020 Feb 27;382(9):845-854. DOI: 10.1056/NEJMra1901593.
Dourmishev, L. A., Dourmishev, A. L. Syphilis: Uncommon presentations in adults. Clin Dermatol. Nov-Dec 2005; 23(6):555-64. DOI: 10.1016/j.clindermatol.2005.01.015.
Çakmak S.K., Tamer E., Karadag A.S., Waugh M. Syphilis: A great imitator. Clinics in Dermatology. 2019; 37, 182–191. DOI: https://doi.org/10.1016/j.clindermatol.2019.01.007
Apoita.Sanz M., González-Navarro B., Jané-Salas E., Marí-Roig A., Estrugo-Devesa A., et al. Sífilis: manifestaciones orales, revisión sistemática. Avances en odontoestomatología. 2020, 36 (3), 161-173. DOI no disponible.
Watts, P. J., Greenberg, H. L., Khachemoune, A. Unusual primary syphilis: Presentation of a likely case with a review of the stages of acquired syphilis, its differential diagnoses, management, and current recommendations. Int J Dermatol. 2016 Jul; 55(7):714-28. DOI: 10.1111/ijd.13206
Leuci S., Martina S., Adamo D., Ruoppo E., Santarelli A., Sorrentino R., et al. Oral Syphilis: a retrospective analysis of 12 cases and a review of the literature. Oral Dis 2013; 19: 738–746. DOI: 10.1111/odi.12058
Drago, F., Ciccarese, G., Cogorno, L., Tomasini, C. F., Cozzani, E. C., Riva, S. F., et. al. Primary syphilis of the oropharynx: an unusual location of a chancre. Int J STD AIDS. 2015 Aug; 26 (9): 679-81. DOI: 10.1177/0956462414551235.
Hernández C., Fúnez R., Repiso B., Frieyro M. Utilidad de la inmunohistoquímica con anticuerpos antitreponema en el diagnóstico de la sífilis. Actas Dermosifiliogr. 2013; 104: 926-928. DOI 10.1016/j.ad.2012.12.011
Ling L., Hui Zi G., Tao W., He Yi Z., Jun L. Primary Syphilis: a histological and immunohistochemical evaluation. Research article. 2020. DOI: https://doi.org/10.21203/rs.2.24783/v1
Murillo E.. Protocolo diagnóstico y tratamiento de las úlceras genitales. Medicine. 2018;12(59):3474-9. DOI no disponible.
Roett M.A.. Genital Ulcers: Differential Diagnosis and Management. Am Fam Physician. 2020 Mar 15;101(6):355-361. PMID: 32163252.
Guidelines for the management of symptomatic sexually transmitted infections. Genital ulcer disease syndrome. Geneva: World Health Organization; 2021 Jun. 10.
Wong T., Singh A.E., De P. Primary syphilis treatment response to doxycycline/tetracycline versus benzathine penicillin. Am J Med. 2008 Oct; 121(10): 903-8. DOI: 10.1016/j.amjmed.2008.04.042.
Janier M., Unemo M., Dupin., Tiplica G.S., Potočnik M., Patel R. 2020 European guideline on the management of syphilis. J Eur Acad Dermatol Venereol. 2021 Mar; 35(3):574-588. DOI: 10.1111/jdv.16946.
Diaz Cuero Y. V., Vidal Cagigas A. Sífilis secundaria: reporte de 2 casos. Rev Asoc Colomb Dermatol. 2019; 27 : 2 (abril - junio), 143-146. DOI no disponible.
Ivars-Lleó, M., Clavo.Escribano, P., Menéndez-Prieto, B. Manifestaciones cutáneas atipícas en la sífilis. Actas Dermo-Sifiliográficas, 2015. 107(4), 275–283. DOI:10.1016/j.ad.2015.11.002
Hook, E. W. Syphilis. Lancet. 2017 Apr 15; 389 (10078): 1550-1557. DOI: 10.1016/S0140-6736(16)32411-4.
Dombrowski J. C. Celum C., Baeten J. Chapter 43. Secondary Syphilis. En: Sanford C.A., Pottinger P.S., Jong E.C. The Travel and Tropical Medicine Manual, fifth Edition, Washington: El sevier; 2017; 535-544. DOI: https://doi.org/10.1016/B978-0-323-37506-1.00043-X
Musher D. M., Baughn R. E. Secondary Syphilitic Lesions. Clin Microbiol Rev. 2005 Jan; 18(1): 205-16. DOI: 10.1128/CMR.18.1.205-216.2005
Hernández-Bel, P., Unamuno, B., Sánchez-Carazo, J. L., Febrer, I., Alegre, V. Alopecia sifilítica: presentación de 5 casos y revisión de la literatura. Actas Dermo-Sifiliográficas. 2013, 104(6), 512–517. DOI: 10.1016/j.ad.2012.02.009
Tognetti L., Cinotti E., Perrot JL., Campoli M., Rubegni P. Syphilitic alopecia: uncommon trichoscopic findings. Dermatol Pract Concept. 2017 Jul 31;7(3):55-59. DOI: 10.5826/dpc.0703a12.
Krase, I. Z., Cavanaugh, K., Curiel-Lewandrowski, C. A case of rupioid syphilis. JAAD Case Reports. 2016, 2(2), 141–143. DOI: 10.1016/j.jdcr.2016.01.006
Braue, J., Hagele, T., Yacoub, A. T., Mannivanan, S., Glass, F., et al. A Case of Rupioid Syphilis Masquerading as Aggressive Cutaneous Lymphoma. Mediterr J Hematol Infect Dis. 2015, 7(1), 2015026. DOI:10.4084/mjhid.2015.026
Liu, X. K., Li, J. Histologic Features of Secondary Syphilis. Dermatology. 2020; 236 (2): 145-150. DOI: 10.1159/000502641.
Who guidelines for the treatment of Treponema pallidum (syphilis). World Health Organization. Geneva, Switzerland. 2016. ISBN 978 92 4 154980 6
Pereira, T. M., Fernandes, J. C., Vieira, A. P., Basto, A. S. Tertiary syphilis. Int J Dermatol. 2007 Nov;46(11):1192-5. DOI: 10.1111/j.1365-4632.2007.03438.x.
Kennedy J.L., Barnard J.J., Prahlow J.A. Syphilitic coronary artery ostial stenosis resulting in acute myocardial infarction and death. Cardiology. 2006;105(1):25-9. DOI: 10.1159/000088337
Moon, J., Yu, D. A., Yoon, H. S., Cho, S., Park, H. S. Syphilitic Gumma: A Rare Form of Cutaneous Tertiary Syphilis. Ann Dermatol. 2018 Dec; 30(6): 749–751. DOI: 10.5021/ad.2018.30.6.749
Musher D.M., Hamill R.J., Baughn R.E. Effect of human immunodeficiency virus (HIV) infection on the course of syphilis and on the response to treatment. Ann Intern Med. 1990 Dec 1;113(11):872-81. DOI: 10.7326/0003-4819-113-11-872.
Charlton, O. A., Puri, P., Davey, L., Weatherall, C., Konecny, P. Rapid progression to gummatous tertiary syphilis in a patient with HIV. Australas J Dermatol. 2019 Feb;60(1):e48-e50. DOI: 10.1111/ajd.12860.
Semblano M. J., Cardoso A., Macêdodo B.A., Haber A., Guimarães M. Nodular tertiary syphilis in an immunocompetent patient. An. Bras. Dermatol. 91 (4) • Jul-Aug 2016 • https://doi.org/10.1590/abd1806-4841.20163837
Berger J.R., Waskin H, Pall L., Hensley G., Ihmedian I. Syphilitic cerebral gumma with HIV infection. Neurology Jul 1992, 42 (7) 1282; DOI: 10.1212/WNL.42.7.1282
Bancroft JD, Stevens A. Theory and Practice of Histological Techniques, 4th edition, Churchill Livingstone Inc., New York, New York, 1996
Belmonte L.P, Táquez A.E., Cerón C.A., Gauto M., Menezes M.V, Miranda A., et.a l. Lesiones atípicas de sífilis terciaria. Rev Asoc Colomb Dermatol. 2012; 20: 4 (Octubre-Diciembre), 370-373. DOI no disponible.
Centers for Disease Control and Prevention. Sexually Transmitted Infections Treatment Guidelines, 2021. Tertiary Syphilis: CDC, fecha de publicación: julio 2022, fecha de consulta: abril 14 2022. Disponible en: https://www.cdc.gov/std/treatment-guidelines/tertiary-syphilis.htm
Cantor A.G., Pappas M., Daeges M., Nelson H.D. Screening for Syphilis: Updated Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA. 2016;315(21):2328–2337. DOI:10.1001/jama.2016.4114
Zhamungui-Sánchez E.F., Herrera-Escobar E.C., Landázuri-González C.R., Vinueza-Mora P.A. Análisis de técnicas treponémicas y no treponémicas en el tamizaje serológico de sífilis. Rev. cuba. hematol. inmunol. hemoter 2017; 33(3): 75-83. tab. ID: biblio-960423
Gayet-Ageron A., Sednaoui P., Lautenschlager S, Ferry T, Toutous-Trellu L, Cavassini M, et al. Use of Treponema pallidum PCR in Testing of Ulcers for Diagnosis of Primary Syphilis. Emerging Infectious Diseases. 2015;21(1):127-129. DOI:10.3201/eid2101.140790.
Henao-Martínez, A. F., Johnson, S. C. Diagnostic tests for syphilis: New tests and new algorithms. Neurol Clin Pract Apr 2014, 4 (2) 114-122; DOI: 10.1212/01.CPJ.0000435752.17621.48
Zhou C., Zhang X., Zhang W., Duan J., Zhao F. PCR detection for syphilis diagnosis: Status and prospects. J Clin Lab Anal. 2019 Jun;33(5):e22890. DOI: 10.1002/jcla.22890.
Cruz, A.R. Diagnóstico de sífilis: al derecho y al revés. Rev Asoc Colomb Dermatol. 2019; 27 : 1 (enero - marzo), 6-11.
How to Cite
Downloads
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Revista de la Asociación Colombiana de Dermatología y Cirugía Dermatológica

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.

| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |






