Hypomelanosis of Ito: a case report
DOI:
https://doi.org/10.29176/2590843X.984Keywords:
Incontinentia pigmenti achromians, pigmentation disorders, Ito syndrome, seizures, mosaicism.Abstract
Hypomelanosis of Ito (HI) is a rare multisystem syndrome considered the third most common neurocutaneous disorder, with a worldwide incidence of 1 in 7,540 newborns.
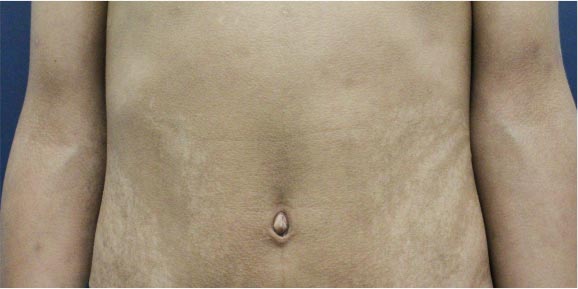
We present the case of a male teenager with a history of a single convulsive episode associated with bilateral hypochromic linear macules, following the lines of Blaschko, present at trunk and extremities since birth.
The diagnosis of hipomelanosis of Ito was based on clinical findings and complementary studies results.
Author Biographies
Mario Alberto Naranjo
Médico dermatólogo; docente, Fundación Universitaria de Ciencias Salud, Hospital de San José, Bogotá, D.C., Colombia
Mauricio Torres
Médico dermatólogo pediatra; docente, Fundación Universitaria de Ciencias de la Salud; director, programa de Dermatología, Fundación Universitaria de Ciencias de la Salud,, Hospital de San José, Bogotá, D.C., Colombia
Myrna B. Gómez
Médica, residente de Dermatología, Fundación Universitaria de Ciencias de la Salud, Hospital de San José, Bogotá, D.C., Colombia
References
Gómez-Lado C1, Eirís-Puñal J, Blanco-Barca O, del Río-Latorre E, Fernández-Redondo V, Castro-Gago M. Hypomelanosis of Ito. A possibly under-diagnosed heterogeneous neurocutaneous syn¬drome. PubMed - NCBI. Rev Neurol. 2004 Feb 1-15;38(3):223-8.
https://doi.org/10.33588/rn.3803.2003618
Ruggieri M, Pavone L. Hypomelanosis of Ito: Cli¬nical syndrome or just phenotype? J Child Neurol. 20 J Child Neurol. 2000 Oct;15(10):635-44
https://doi.org/10.1177/088307380001501001
Park JM, Kim HJ, Kim T, Chae HW, Kim DH, Lee MG. Sexual precocity in hypomelanosis of Ito: Mosaicism-associated case report and literature review. Int J Dermatol. 2011;50:168-74.
https://doi.org/10.1111/j.1365-4632.2010.04639.x
Romero A, Salazar M, Tufino M, Villacís A, Ga¬larza F. Hipomelanosis de Ito. Dermatol Rev Mex. 2015;59:43-8.
Pascual-Castroviejo I, Roche C, Martínez-Bermejo A, Arcas J, López-Martín V, Tendero A, et al. Hy¬pomelanosis of Ito. A study of 76 infantile cases. Brain Dev. 1998;20:36-43.
https://doi.org/10.1016/S0387-7604(97)00097-1
Ream M. Hypomelanosis of Ito. Handb Clin Neurol. 2015;132:281-9.
https://doi.org/10.1016/B978-0-444-62702-5.00021-4
Ruiz-Maldonado R, Toussaint S, Tamayo L, Laterza A, del Castillo V. Hypomelanosis of Ito: Diagnostic criteria and report of 41 cases. Pediatr Dermatol. 1992;9:1-10.
https://doi.org/10.1111/j.1525-1470.1992.tb00317.x
Kouzak SS, Mendes MS, Costa IM. Cutaneous mo¬saicisms: Concepts, patterns and classifications. An Bras Dermatol. 2013;88:507-17.
https://doi.org/10.1590/abd1806-4841.20132015
Pavone V, Signorelli SS, Praticò AD, Corsello G, Savasta S, Falsaperla R, et al. Total hemi-over¬growth in pigmentary mosaicism of the (hypome¬lanosis of) Ito type: Eight case reports. Medicine (Baltimore). 2016;95:e2705.
https://doi.org/10.1097/MD.0000000000002705
Taibjee SM, Bennett DC, Moss C. Abnormal pig¬mentation in hypomelanosis of Ito and pigmen¬tary mosaicism: The role of pigmentary genes. Br J Dermatol. 2004;151:269-82.
How to Cite
Downloads
Downloads
Published
How to Cite
Issue
Section

| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |






